Image 1 of 2
Image 1 of 2

 Image 2 of 2
Image 2 of 2



SLP Postural & Breathing Checklists for Voice Evaluations (Digital Download)
Purpose of This Resource
This digital download includes two essential clinical tools for voice evaluations: the SLP Postural Checklist and the SLP Breathing Checklist. Designed for speech-language pathologists, these resources identify postural imbalances and respiratory patterns that may contribute to voice disorders or impede recovery. Together, they support a holistic approach to voice therapy by addressing biomechanical and physiological factors often overlooked in standard assessments.
Why It Matters
Voice production relies heavily on the efficient coordination of posture and respiration. Disruptions in either area can lead to increased muscular tension, reduced breath support, and compensatory behaviors that perpetuate dysphonia. These checklists provide clinicians with a structured method to assess these foundational elements, revealing contributing factors that influence onset, persistence, or recurrence of voice issues.
What’s Included
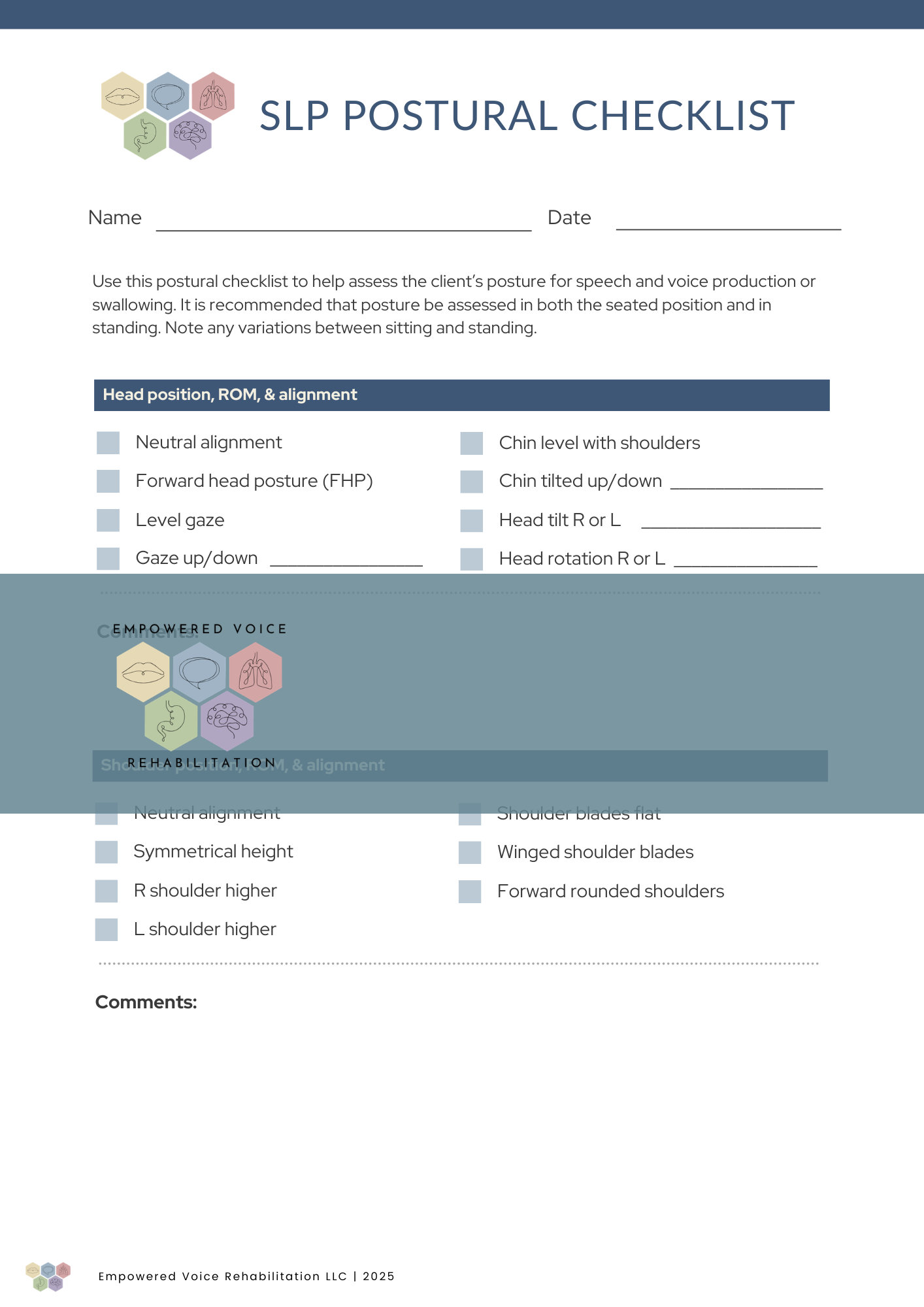
SLP Postural Checklist: A 2-page clinician observation tool designed to evaluate static and dynamic alignment, muscle tension patterns, and musculoskeletal factors that directly impact the vocal mechanism.
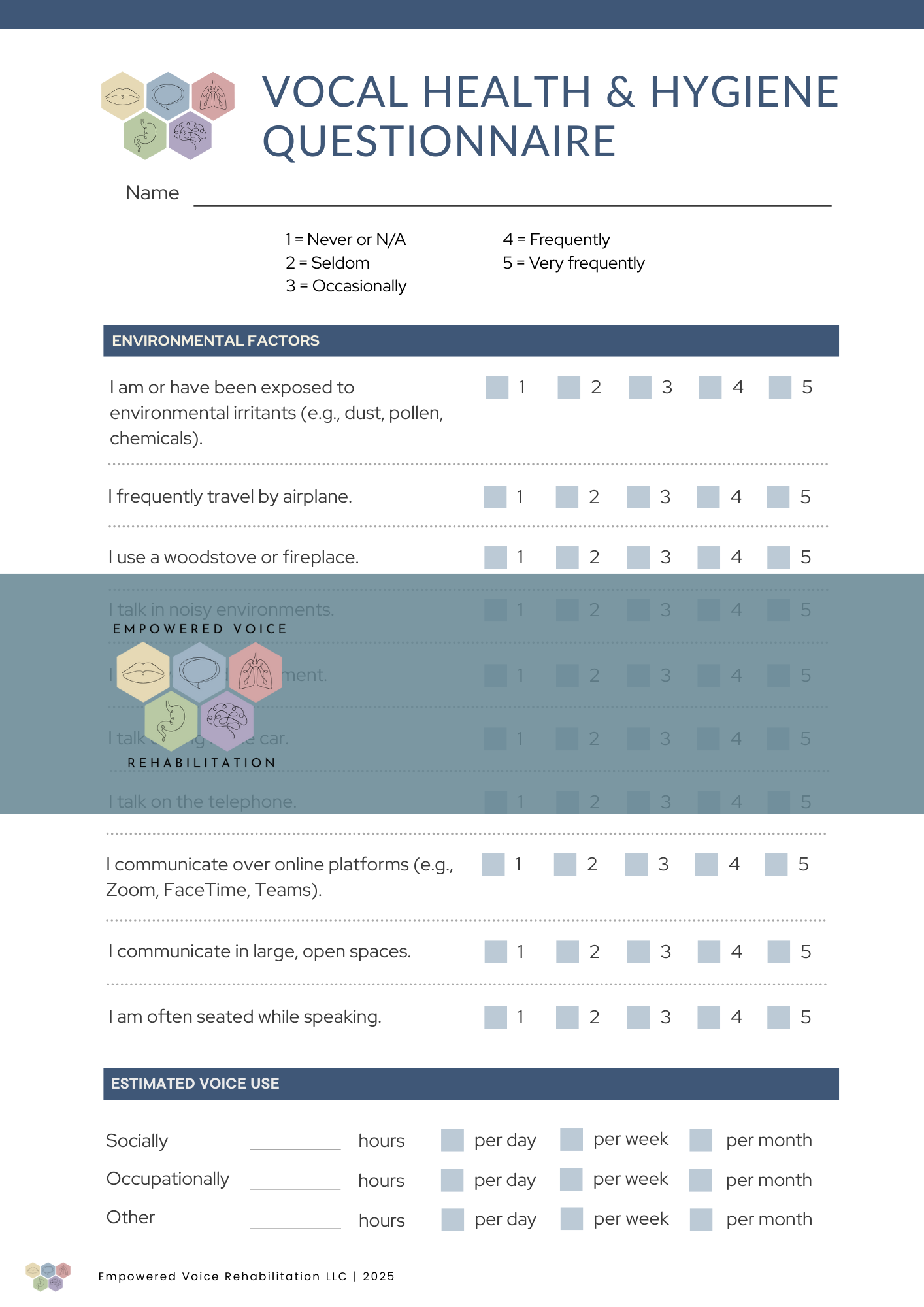
SLP Breathing Checklist: A 1-page comprehensive clinical assessment guide focusing on respiratory patterns, breath support efficiency, and the coordination of respiration necessary for phonation and voice stamina.
How to Use This Tool
Initial Evaluation: Administer the checklists during the first sessions to establish a baseline of the client’s postural alignment and respiratory function.
Identify Contributing Factors: Use the clinician observations to pinpoint specific biomechanical or respiratory patterns that may be exacerbating voice disorders or limiting recovery.
Guide Therapy Planning: Translate findings directly into targeted interventions, such as specific postural realignment exercises or breath support strategies.
Monitor Progress: Re-administer the checklists periodically to track changes in alignment and breathing efficiency, allowing for data-driven adjustments to the treatment plan.
Important Note
These checklists serve as clinical observation tools to inform voice therapy planning. They are not stand-alone diagnostic instruments. While they highlight potential biomechanical and respiratory risk factors, final clinical decisions and diagnoses should always be integrated with instrumental assessments (e.g., laryngoscopy, videostroboscopy), patient history, and professional clinical judgment.
Purpose of This Resource
This digital download includes two essential clinical tools for voice evaluations: the SLP Postural Checklist and the SLP Breathing Checklist. Designed for speech-language pathologists, these resources identify postural imbalances and respiratory patterns that may contribute to voice disorders or impede recovery. Together, they support a holistic approach to voice therapy by addressing biomechanical and physiological factors often overlooked in standard assessments.
Why It Matters
Voice production relies heavily on the efficient coordination of posture and respiration. Disruptions in either area can lead to increased muscular tension, reduced breath support, and compensatory behaviors that perpetuate dysphonia. These checklists provide clinicians with a structured method to assess these foundational elements, revealing contributing factors that influence onset, persistence, or recurrence of voice issues.
What’s Included
SLP Postural Checklist: A 2-page clinician observation tool designed to evaluate static and dynamic alignment, muscle tension patterns, and musculoskeletal factors that directly impact the vocal mechanism.
SLP Breathing Checklist: A 1-page comprehensive clinical assessment guide focusing on respiratory patterns, breath support efficiency, and the coordination of respiration necessary for phonation and voice stamina.
How to Use This Tool
Initial Evaluation: Administer the checklists during the first sessions to establish a baseline of the client’s postural alignment and respiratory function.
Identify Contributing Factors: Use the clinician observations to pinpoint specific biomechanical or respiratory patterns that may be exacerbating voice disorders or limiting recovery.
Guide Therapy Planning: Translate findings directly into targeted interventions, such as specific postural realignment exercises or breath support strategies.
Monitor Progress: Re-administer the checklists periodically to track changes in alignment and breathing efficiency, allowing for data-driven adjustments to the treatment plan.
Important Note
These checklists serve as clinical observation tools to inform voice therapy planning. They are not stand-alone diagnostic instruments. While they highlight potential biomechanical and respiratory risk factors, final clinical decisions and diagnoses should always be integrated with instrumental assessments (e.g., laryngoscopy, videostroboscopy), patient history, and professional clinical judgment.